Globally, women in labour are overtreated. The consequences are dire
Too many women receive oxytocin augmentation and undergo cesarean sections, exposing both women and children to unnecessary risks, a new analysis concludes. The prevalence of overtreatment is shocking, say the researchers behind the analysis.
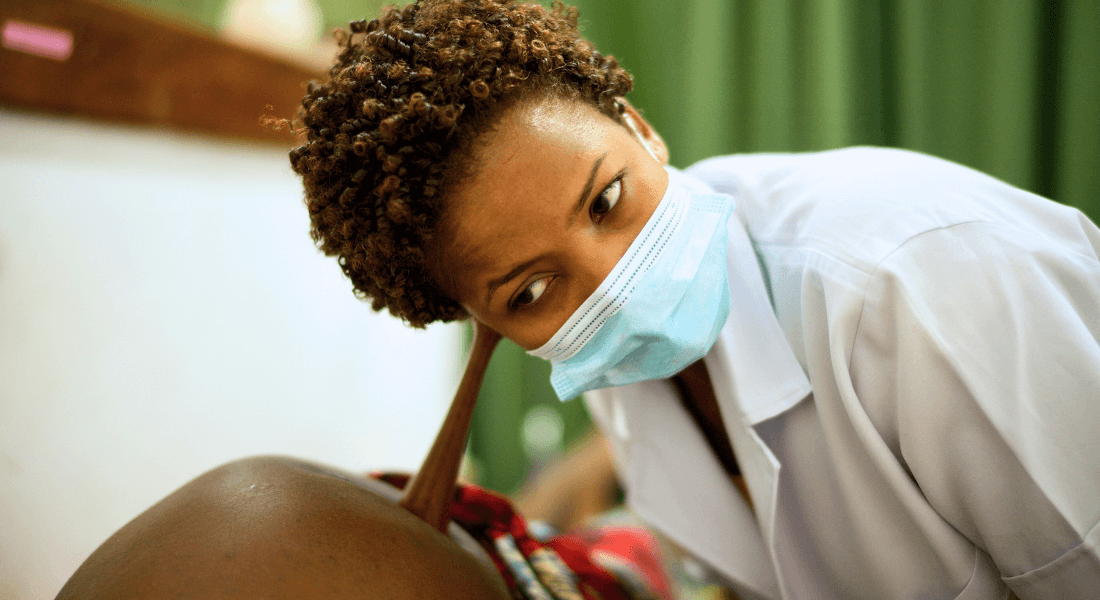
There are approximately 130 million births per year. A substantial proportion of the women giving birth are treated with oxytocin or undergo caesarean sections.
But not all the women receiving treatment actually need it, and overtreatment can be dangerous, a new analysis published in one of the world's leading medical journals, the British Medical Journal, shows.
It is a ‘horror story’ – the fact that we still know so little about oxytocin for augmenting labour, even though it has been used increasingly over the past 70 years
Two of the researchers behind the study are Assistant Professor Nanna Maaløe from the Department of Public Health at the University of Copenhagen and Postdoc Natasha Housseine from the same department and Aga Khan University in Tanzania.
They both emphasise that the global prevalence of overtreatment is shocking considering the fact that a lot of the women do not need the treatment.
In collaboration with Danish and international colleagues, the researchers conducted a comprehensive analysis, mapping research on childbirth with a focus on lack of progress during labour.
"During birth, it is common to see a period of slow or no progress in labour. This is often treated with a drip containing oxytocin to try and boost contractions, and it may result in a caesarean section," Nanna Maaløe explains.

However, the new analysis indicates that while about 10-15 per cent of first-time mothers have a longer-than-expected labour, 30-90 per cent of first-time mothers receive medical augmentation with oxytocin to boost contractions in hospitals worldwide.
And globally, caesarean birth rates are rising fast. In countries such as Turkey, Egypt and Brazil, there are now more caesarean births than vaginal births.
An overlooked pandemic of caesarean sections
Between 2010 and 2018, an average of 21 per cent of women giving birth had caesarean sections. This figure is expected to rise to over 28 per cent by 2030.
When a caesarean section is performed for medical reasons, it can be lifesaving and is an essential part of emergency care during birth. But a caesarean section also carries risks, and whether the surgery is medically indicated must be carefully considered.
"A caesarean section is a major surgery in the uterus and abdominal cavity, with risks of bleeding, infection and prolonged pain. In addition, the caesarean section makes subsequent pregnancies and births riskier because of scarring on the uterus," says Nanna Maaløe.
She emphasises that the risk associated with the procedure is quite low in high-income countries, but in other parts of the world, especially in sub-Saharan Africa, it is much more dangerous.
In many sub-Saharan African countries, it is estimated that about eight per cent of children and approximately one in 100 women die during or shortly after a caesarean section.
"While there is a different risk profile in sub-Saharan Africa than in high-income countries, unnecessary surgery is concerning in all parts of the world. Lack of progress in labour is the most common reason for a woman's first caesarean section, and the timely diagnosis and treatment of this must be improved to break this vicious cycle. It is a central issue in women's health," Natasha Housseine adds.
What we don't know about oxytocin used to stimulate contractions
Oxytocin is used to boost contractions, often with the goal of ultimately avoiding caesarean sections. But there is very little research showing that it actually works.
"As we see with unnecessary caesarean sections, there are risks associated with labour augmentation with oxytocin, which disproportionately affects hospitals with the fewest resources the most. At the same time, we know very little about whether oxytocin helps to avoid caesarean sections," says Nanna Maaløe.
"It is a ‘horror story’ – the fact that we still know so little about oxytocin for augmenting labour, even though it has been used increasingly over the past 70 years and is now provided to 30-90 per cent of first-time mothers in the world’s hospitals," says Nanna Maaløe.
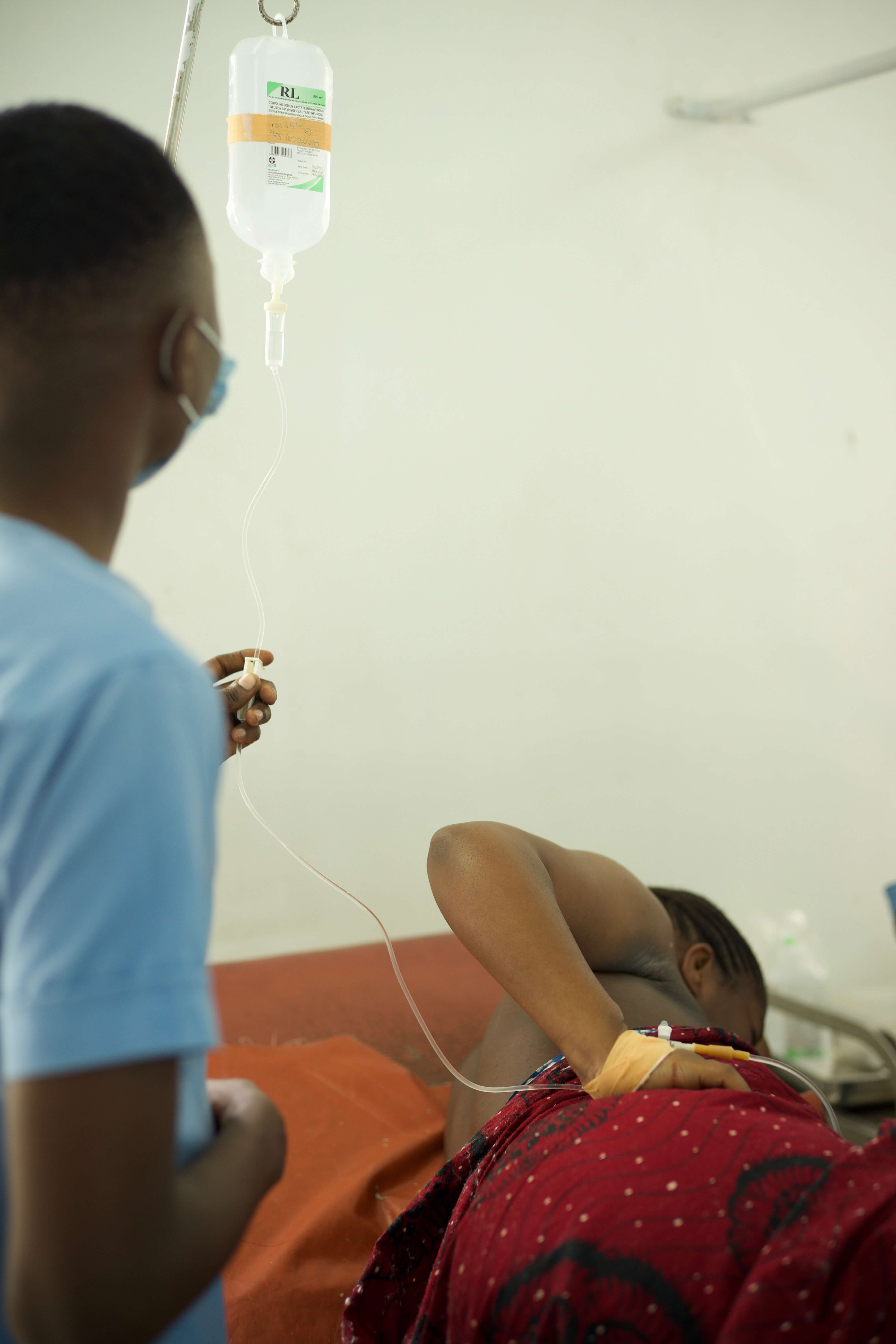
Nanna Maaløe adds that the lack of research on the uterine muscle’s function during labour sharply contrasts with, for example, research done on the skeletal muscles of elite athletes.
"While the treatment of muscle fatigue caused by acid-base changes has been a growing research area in sports medicine since the 1930s, there has been remarkably little exploration of the causes and treatment of uterine muscle fatigue during childbirth," says Nanna Maaløe.
Oxytocin for stimulating contractions causes the uterus to contract more forcefully and frequently, which can result in insufficient blood flow through the umbilical cord. Thus, there is a risk that the baby does not receive enough oxygen.
In the worst cases, this can lead to stillbirths and brain damage in the baby. This is supported by a PhD study by co-author Monica Lauridsen Kujabi.
In high-income countries, oxytocin for stimulating contractions is associated with much less risk for women giving birth. However, the analysis does highlight results from Swedish studies suggesting that during births in Sweden lasting less than 12 hours, the risk of the baby showing signs of oxygen deficiency during birth was higher if the mother had received oxytocin to boost contractions.
"There is a disconnect between best knowledge and practice"
According to Nanna Maaløe and Natasha Housseine, there are several explanations for the large discrepancy between what research suggests that pregnant women need and the treatment they receive.
A central explanation is likely cultural and habitual practices, on the one hand, and a lack of prioritisation of research, on the other.
"Oxytocin was approved for use in high-income countries in the 1950s. At that time, randomised trials were not done prior to approval of such medication. And the crucial function of oxytocin in averting life-threatening bleeding after childbirth likely fostered a particularly favourable perception of the medication. It may be that oxytocin can reduce the number of caesarean sections, if the right women are treated. However, since then, research on the progress of childbirth and related treatment has been deprioritised," Nanna Maaløe explains.
Another possible explanation for the gap between what we know scientifically and what we do may be the congestion and staff shortages in many maternity units worldwide. There is often not enough capacity, so patients need to be ‘processed’ quickly during birth.
"While we do not know if oxytocin leads to fewer caesarean sections, we do know that the drug shortens the duration of labour. And our colleague, Monica Kujabi, has shown in her PhD study that the use of stimulating drops is increasing in busy maternity units in some cities of Africa. This is a form of 'crowd control'," says Natasha Housseine.
Data from Sweden likewise suggest that use of oxytocin for boosting contractions increases when maternity units are busy.
Nanna Maaløe further points to outdated and imprecise clinical guidelines as a reason for this overtreatment. For instance, a woman's first childbirth typically progresses more slowly than stated in many clinical guidelines.
"Naturally, it leads to overtreatment if clinical guidelines are not updated with the latest research. Fundamentally, our analysis suggests that there is an urgent need globally for maternity units with a calm and safe environment supporting the body's natural progress in childbirth – and for the safe use of stimulating drops, when necessary," says Nanna Maaløe, adding:
"Healthcare professionals worldwide need national and global clinical guidelines for childbirth, including timely use of oxytocin and caesarean sections, to be based on the best scientific knowledge in the field. At present, there is a disconnect between best knowledge and practice, and that is unacceptable for the health of women and children."
You can read the analysis "Inconsistent definitions of labour progress and over-medicalisation cause unnecessary harm during birth" in BMJ.
Contact
Assistant Professor Nanna Maaløe
nannam@sund.ku.dk
+4541271984
Postdoc Natasha Hosseine
natasha.housseine@sund.ku.dk
Journalist and press officer Liva Polack
liva.polack@sund.ku.dk
+45 35 32 54 64
