Pregnant women and their unborn babies can die of malaria. Vaccine may be on the way
Malaria is a major health challenge especially in sub-Saharan Africa. Pregnant women and their unborn babies in particular are affected by the parasite. But now a team of researchers has received DKK 75 million in funding for a project that may lead to a vaccine.
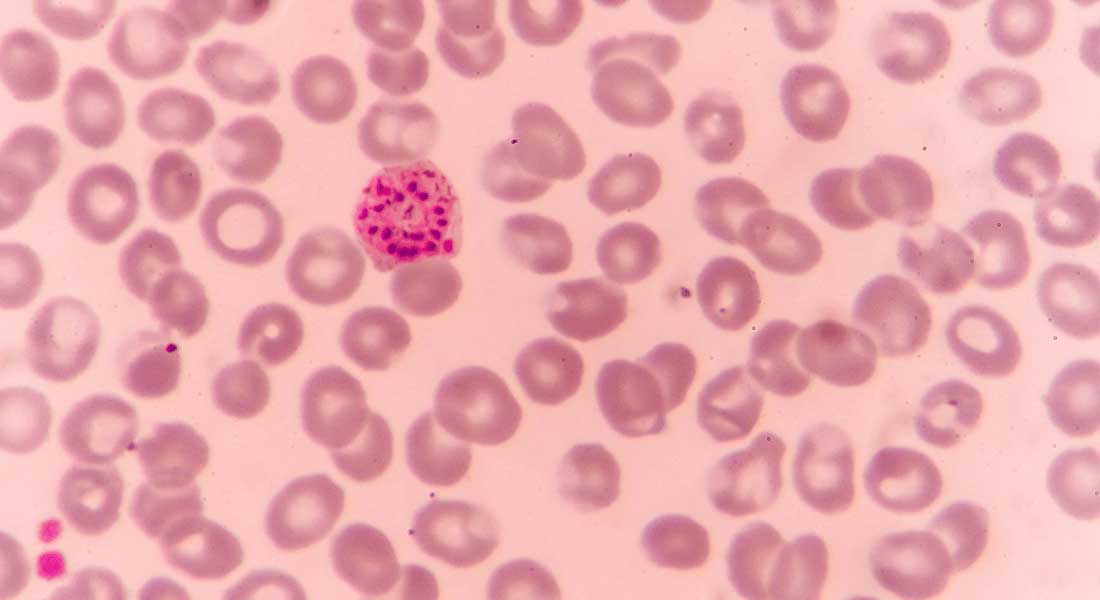
A high fever, tremors and influenza-like symptoms.
Each year, more than 100 million pregnant women are infected with malaria. As many as 50,000 die, and 200,000 lose their baby.
The children that do survive are often underweight, because the malaria parasite infects the placenta and creates a barrier between mother and child, cutting the baby off from nutrients.
Malaria in pregnant women is a huge problem in sub-Saharan Africa – as well as in South America and South Asia. Though the disease can be treated, it requires high-tech hospitals, and not all countries have them.
Now researchers from the University of Copenhagen and Mali, Ghana and Benin, among others, have received DKK 75 million in funding for a project that aims to develop a new malaria vaccine for pregnant women. The funding comes from the EU programme Horizon Europe.
“This gives us a chance to continue our work, and hopefully it will contribute to preventing placental malaria. A vaccine will not solve all our problems, but it can be part of the solution – together with mosquito nets, early treatment and population-wide prevention,” says Associate Professor of Parasitology Morten Agertoug Nielsen and adds:
“The past 50 years, scientists and companies have tried to develop a vaccine for malaria. We hope to be able to finalise their work and develop a vaccine that targets the part of the parasite causing the disease,” he adds.
New vaccine technology is key
In a previous project, Morten Agertoug Nielsen and Professor of Translational Microbiology Ali Salanti produced a malaria vaccine in the form of a soluble protein. The vaccine was based on the ‘hook’ which malaria parasites use to attach to the placenta.
“Unfortunately, the results were not good enough to warrant further human testing. Vaccines based on soluble proteins are generally problematic,” says Morten Agertoug Nielsen.
Associate Professor Adam Sander from the Department of Immunology and Microbiology has therefore spent the past five years heading a project to transform proteins into virus-like particles.
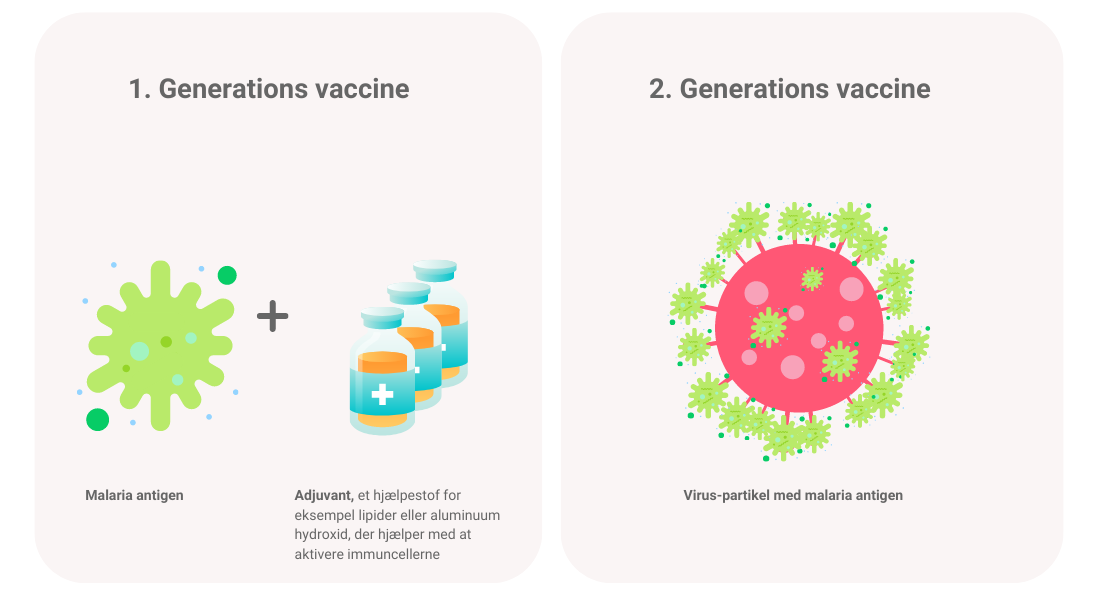
“We believed we had to develop a second-generation vaccine. This vaccine is based on a virus particle,” says Morten Agertoug Nielsen.
By attaching a small amount of malaria to the virus, the vaccine will help the body recognise malaria the first time it is infected with it.
“Immune cells quickly respond to virus particles, realising that this is dangerous. Evolution has taught us that. You do not get the same response when the body is injected with something that is soluble,” Morten Agertoug Nielsen explains.
The researchers will spend the next one-two years developing the vaccine. And according to Morten Agertoug Nielsen, it will take seven to 10 years before they may be able to bring an actual vaccine into the market.
Dreaming of an all-round malaria vaccine
Malaria spreads in ever-widening circles in the countries worst affected by the disease. Aside from pregnant women and unborn babies, other children and adults are affected too.
The WHO estimates that 241 million people were infected with the disease in 2020. More than 600,000 died, most of whom were children living in Africa.
“In general, malaria has a huge negative effect, especially on the African continent. Aside from the tragedy of the many deaths, especially among children, people suffering from malaria get very sick and are therefore unable to work. So the socio-economic effects of the disease are substantial too,” Morten Agertoug Nielsen says and adds:
“Our dream is to continue to work on the vaccine we are developing right now and create an all-round malaria vaccine for everyone using the same technology.”
Contact
Associate Professor Morten Agertoug Nielsen
mortenn@sund.ku.dk
+45 35 32 68 03
Journalist and press consultant Liva Polack
liva.polack@sund.ku.dk
+45 35 32 54 64
